The bones that form our skeletal system are hard enough to provide us with support to enable walking, and other functions without the fear of them breaking.
Nevertheless, under traumatic conditions bones can break and cause what is known as a fracture. Of course, for this to happen there must be a situation in which immense pressure is exerted on them such as in high impact blows after accidents, falls, or violence. On rare occasions it can happen automatically after a small lesion that can evolve into a fracture.
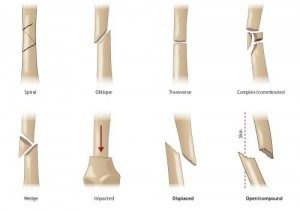
Fractures can be partial or total, in other words, with a lot of fragments scattered around and possible displacement of the bones.
They always exhibit acute pain, a sense of burning, distortion of the area, swelling, heat and dysfunction. The patient needs to keep the injured part of the body immobile, otherwise every movement will cause pain.
Diagnosis of a fracture by an experienced orthopaedic surgeon is rather easy, although an x-ray should be performed in order to verify and categorize the fracture.
This way, with the correct X-ray images the treatment can be determined. In other words, whether the treatment is going to be conservative (cast, plaster, immobilization) or surgical.
Following x-ray imaging inspection, the fracture can be categorized. Many criteria determine whether or not a surgical operation will be required:
- age
- displacement of the fracture
- number of fractured fragments
- daily needs
- coexisting health conditions
By the term fracture displacement, which is a very important factor in decision making as well as the surgical method, we mean the gap between fractured fragments and the deviation from the normal anatomic structure of the bones.
The first thing that needs to be taken care of is the immobilisation of the broken limb (upper or lower extremity) or the part of the body that is suspected to have been fractured (spine, pelvis) and the transportation to an orthopaedic clinic for further investigation.
Fractures that meet the criteria for conservative treatment are dealt with external aids (slings, plaster casts, braces, bed-rest). Patients with fractures that meet the criteria for surgical treatment need to be hospitalized and operated on as soon as possible.
Dealing with a fracture immediately using either method relieves the patient’s initial pain and prevents complications that can appear even a few hours after of the injury.
The healing of fractures is a time consuming process and both the patient and the orthopaedic surgeon ought to cooperate and exercise patience.
 In orthopaedic pathology, with the term upper extremity, we refer to the anatomical area that extends from the shoulder to the tips of the fingers. It comprises the shoulder joint with its surrounding tendons, the humerus with its muscles, the elbow joint, the antibrachium, the area of the wrist and finally the fingers.
In orthopaedic pathology, with the term upper extremity, we refer to the anatomical area that extends from the shoulder to the tips of the fingers. It comprises the shoulder joint with its surrounding tendons, the humerus with its muscles, the elbow joint, the antibrachium, the area of the wrist and finally the fingers.
The pathology of the upper extremity can exhibit numerous conditions, acute as well as chronic. An acute condition can be an inflammation or a fracture, while a chronic one can be a degenerative condition (deterioration) such as tendonitis and arthritis.
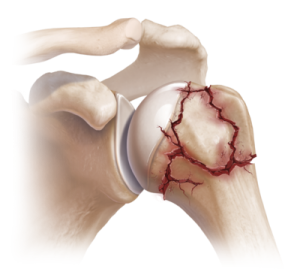
Proximal Humerus fracture
With the term proximal humerus fracture we refer to the area of the shoulder, and more specifically the head of the arm bone (humerus) that joins the shoulder called the glenohumeral joint.
The area of the shoulder exhibits a dense coverage of muscles that firmly stabilize the head to the glenoid. Nerves and blood vessels which lead to the upper limb for sensitivity and haematosis are routed through the area of the armpit.
A fracture in this area almost always occurs after a fall from a standing position, and after an x-ray is classified depending on the number of fractured fragments and its dislocation.
Therefore, the number of fragments (two, three or four) and their dislocation, i.e. how far they are dislocated from each other, will determine not only the type of treatment (conservative or surgical) but also the prognosis of the outcome, good or bad.
The clinical indications of the fracture are: acute pain, swelling, hematoma, bruising, inability of movement due to pain, specifically the patient supports the fractured arm with the healthy one.
After the x-ray it’s time for treatment, which is usually conservative. In other words, placing the fractured arm in a sling.
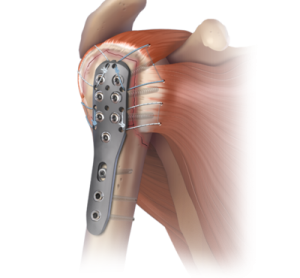
With fractures that display dislocation larger than the anatomically accepted limits, a surgical approach is necessary with the so called internal osteosynthesis that includes wires, diadermic needles, plates and screws. When shattering is extensive, i.e. a four piece fracture in which the survival of the femoral head is in danger of necrosis, another surgical operation takes called arthroplasty takes place. This involves the exchange of the shattered head with a new metal one.
It needs to be mentioned that the choice of therapy is multifactorial. This means that the doctor has to take a lot of factors into consideration, such as, the age of the patient, the dominant arm (right or left handed), the patient’s daily needs and any coexisting health problems.
The results are normally positive, either with conservative or surgical treatment. In conjunction with the healing of the fracture and positive x-ray results, a physiotherapy programme is followed, to avoid the stiffness that follows an injury of the arm.
After a few weeks the fracture is considered healed (bonded) and after a few months is back to normal.
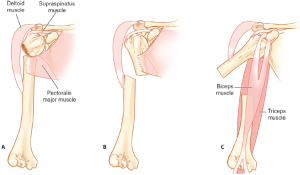
FRACTURE OF THE HUMERAL SHAFT
Humeral shaft fractures refer to the ones in the area between the humerus head and the elbow. They are classed the same way as other luminal bones into transverse, spiral or comminuted.
They usually occur after a fall and their clinical indications are the inability of movement of the arm in any way, swelling, hematoma and acute pain. The patient supports the fractured arm with the healthy one.
Clinical examination and an x-ray should always be performed in order to exclude nerve and blood vessel damage. The x-ray will determine the extent of the fracture and therefore the treatment required.
Treatment can be conservative, in other words with the application of a cast, or surgical. There are a lot of criteria that determine whether a surgical operation is required, and a lot of parameters must be taken into account, such as the patient’s age, the daily activities undertaken and the type of fracture.
A surgical operation ensures stabilisation of the fracture with osteosynthesis materials (plates, screws, nails) and the immediate mobilization of the arm.
FRACTURES OF THE FOREARM AND THE WRIST
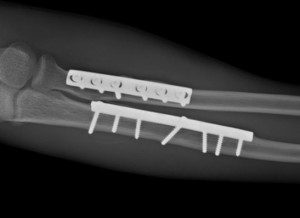
Fractures of the forearm concern the radius and the ulna. They can occur either to one or both bones at the same time.
Only on rare occasions are they dealt with conservatively, i.e. with plaster, so the majority of patients need to undergo surgery. Osteosynthesis materials used are a plate and screws, in order to ensure stability of the fracture and quick healing.
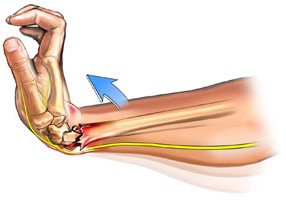
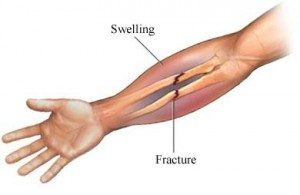
Fractures of the wrist or the styloid process of radius are a common occurrence. They usually happen to the elderly due to osteoporosis or after a fall from standing position. They are intra or extra joint fractures. The majority of them are away from the joint as far as the clinical indications the patient complains of acute pain, inability of hand movement, deformation of the area and swelling.
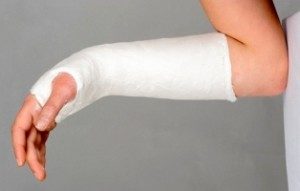
As always the next step is an x-ray of the area and the classification of the fracture. Typically, these fractures are dealt with conservatively, in other words, with immediate resetting of the bones after local anaesthesia and with the application of plaster from the elbow to the fingers.
In some cases, a surgical operation is needed, mainly when the fractures involve the wrist joint as well.
The fractured arm remains in plaster for a few weeks followed by a rehabilitation program.
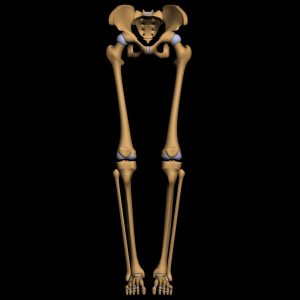
The term lower extremity anatomically refers to the area starting from the hip joint, includes the femur, the knee with its ligaments, the ankle joint and finishes at the end of the foot with the toes.
As with the upper extremity the pathological conditions can be chronic or acute.
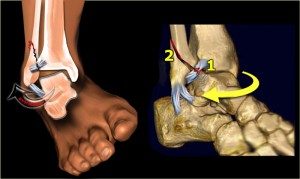
LATERAL AND MEDIAL MALLEOLUS FRACTURES
The term malleolus refers to the area of the end part of the fibula, the lateral (outer), and the end part of the tibia that surrounds the ankle, the medial (inner).
In general, particular attention needs to be paid when dealing with malleolus fractures. They can soon exhibit swelling and if the orthopaedic surgeon does not take immediate action, air pockets appear on the skin exactly in the area of the fracture making the surgical operation complicated and unsafe.
We can have isolated fractures of the lateral malleolus, the medial malleolus or bimalleolar ones. It needs to be pointed out that almost always ligament damage coexists with the fractures and needs to be taken into consideration during their surgical confrontation.
On rare occasions treatment is conservative, with the application of plaster or a cast but almost always the bone is successfully reset only surgically. A perfect reset is necessary and internal osteosynthesis with a plate and screws.
The most frequent complications that appear in these fractures are as previously mentioned: air pockets, necrosis of the skin, unsuccessful reset, instability, stiffness of the ankle that restricts movement, post traumatic arthritis, chronic swelling, inflammation and vein thrombosis of the lower limb.
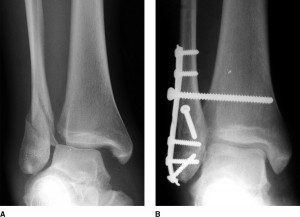
Fractures of the tibia from the centre to the outer of the bone:
- fractures of the tibial plateau
- fractures of the shaft
- fractures of the bottom 1/3 of the tibia (pilon)
The fractures of the tibial plateau are intra joint fractures, in other words they refer to part of the joint. Therefore, their treatment should be optimal in order to avoid damage to the joint. The aim of the treatment is the safeguarding of integrity of the joint through a stable osteosynthesis process. Any disruption of the integrity of the joint may result in post- traumatic arthritis with negative effects on the patient’s daily activities. They are very demanding fractures as far as their confrontation, but with the correct method a patient can be guaranteed stability and a quick return to daily life.
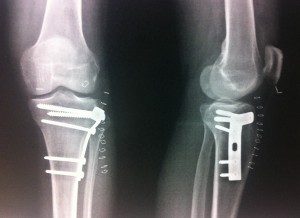
Fractures of the femoral area refer to the shaft and the lower 1/3 of the bone. Therefore, they are fractures of the shaft as well as epicondyles. Shaft fractures occur on the luminal part of the bone, while those epicondyles ones occur in the area of the knee and above it.
They are serious lesions with a lot of blood loss and they are rarely dealt with conservatively. They occur after high energy collision lesions and are more often seen in younger individuals.
Clinically, they display extensive swelling of the thigh, due to the large amount of blood around the injured bone, leg shortening, acute pain after each movement whether, active or passive and inability to walk.
After the patient’s admission to an orthopaedic clinic the injury is evaluated and an x-ray is performed to identify the type of fracture.
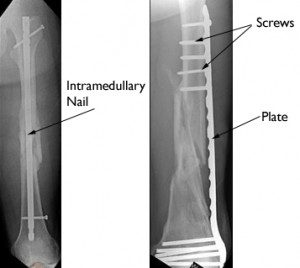
As previously mentioned the treatment of the fracture is surgical. An internal osteosynthesis is performed with the use of a plate with screws or a metal rod within the bone through a small incision on the skin. This is known as intramedullary nailing.
The patient leaves hospital with advice on care of the leg and prescribed medication (anticoagulants and painkillers).
The intertrochanteric fracture is the most common fracture that happens to the elderly after a fall from a standing position.
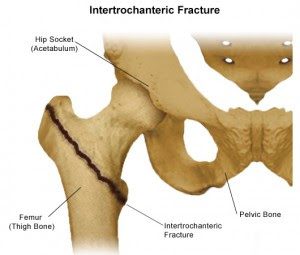
Anatomically we refer to the area of the hip, and specifically the area between the femoral head and the shaft.
It is a serious lesion and usually occurs to the elderly due to osteoporosis.
Clinically, after the fall the patient is unable to stand or walk and is lying on the floor usually with the injured leg deformed (shorter than the other) and with an external rotation (the leg turns outwards). Any attempt to move causes severe pain and therefore the patient remains immobile.
Diagnosis by an experienced orthopaedic surgeon is clinical, in other words the pain in the area of the hip with a distortion of the lower limb that bares the fracture as well as the difficulty of any sort of movement of the lower limb by the patient or the doctor, make the doctor suspect a fracture.
There is an urgent need for the patient to be transported to a clinic. A correct imaging test will verify the fracture and the orthopaedic surgeon will class it. The classification of the fracture, in other words the number of fragments and the area of the fracture, will determine the form of treatment.
The treatment is almost always surgical and it is performed with internal osteosynthesis by placing implants depending on the morphology of the fracture.
The materials used are a plate with screws (percutaneous pinning) and intramedullary nailing.
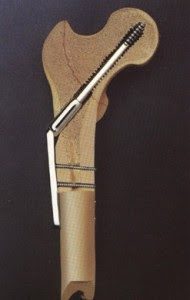
Richard DHS Plate

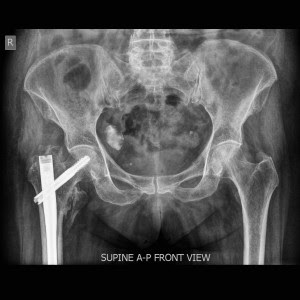
Intramedullary Nail
After the preoperative tests and the provision for 2-3 units of blood, the patient is taken to theatre and the operation is then performed under epidural or total anaesthesia.
With x-ray assistance the reset of the fracture is done followed by internal osteosynthesis. In a case where intramedullary nailing is necessary, the implants are inserted through 3 small incisions and then fitted. Blood loss during the operation is minimal and the time in theatre is brief.
After surgical stabilization of the fracture, the patient is able to sit up in bed the next day and the following day is able to take their first few steps with the aid of a physiotherapist.
The patient stays in the clinic 4-5 days and is then discharged with a rehabilitation program to follow and medication (anticoagulant injections, painkillers)
All patients, apart from a few exceptions, must be operated on. This way the patient will walk as he used to and complications due to bed- rest that can occur from the first day such as: infection of the respiratory system, vein thrombosis of the lower limbs, bedsores and pneumonic embolism will be prevented.
Surgery should not be performed if the patient suffers from bone cancer in the final stages, decompensated heart failure in the final stages or an active infection of any sort.
The femoral neck fracture is one of the most common fractures in the elderly and refers to the hip area. It occurs in younger individuals as well, usually after high energy collision injuries, such as road traffic accidents. More specifically it occurs under the femoral head, which is why it is called the femoral neck.
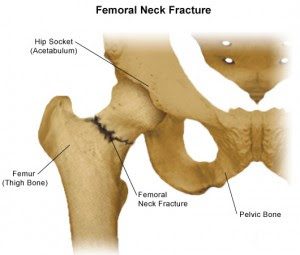
It occurs after the patient has fallen from standing position and makes the patient immobile. Every movement of the lower limb is painful mainly around the area of the hip.
After clinical examination of a suspected fracture, the patient must be sent to an orthopaedic clinic for x-ray examination.
The diagnosis, the classification of the fracture after the x-ray as well as the age of the patient will determine the type of treatment, which is almost always surgical.
The anatomical position of the fracture (acetabulum (hip socket) fracture – a fracture that is surrounded by synovial fluid) as well as the peculiarity of haematosis of the femoral head, make healing of the fracture uncertain and therefore surgical confrontation is essential. This means that the femoral head is in danger of necrosis and is almost always is replaced by an alloy one.
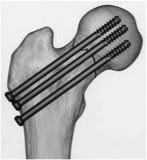
When a patient is young the replacement of the femoral head with an artificial one is not desirable due to future complications. Therefore, the surgeon attempts to reset it and stabilise it by fitting 3 screws. Although the femoral head is supported by 3 screws, it is susceptible to shifting and damage of haematosis so, the patient must be monitored for possible necrosis and the collapse of the head at frequent intervals over a two year period.
With elderly patients it is rare to stabilise the femoral head with screws, so another operation is performed called arthroplasty (partial or total arthroplasty).
In the latter case, the fractured femoral head is removed and an implant with an alloy head on its end is inserted into the femur, which along with the acetabulum will form the new joint.
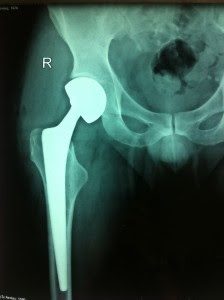
Partial Arthroplasty of the Hip
In this operation 3 units of blood are needed. It is performed under epidural or total anaesthesia and lasts about an hour and a half.
The next day the patient is able to sit up in bed and the following day is able to take their first few steps with the aid of a physiotherapist. The patient stays in the clinic for 5 days and is then discharged with a rehabilitation plan.
Due to the nature of the operation, extreme movements of the joint should be avoided during the first few weeks to avert dislocation of the hip. Special equipment is fitted to raise the height of the patient’s bed and toilet. The patient is able to walk without fear and takes anticoagulant medication for 30 days.
