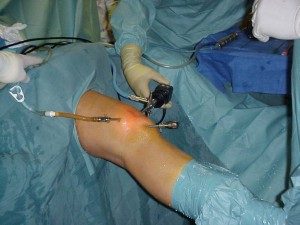
Arthroscopy is an operation in which the orthopaedic surgeon, with the help of a special microscopic camera a few millimetres in diameter, is able to observe the internal workings of a joint.
With an arthroscopy an orthopaedic surgeon can diagnose and treat intra articular disorders.
A special light source with a camera is routed through a wire into the joint and the images are projected onto a monitor which the Surgeon observes while performing the operation. With a special pump, a controlled flow of saline solution is injected into the joint to expand it and allow the Surgeon to operate more easily.
With the arthroscopy method the Surgeon is able to inspect the integrity of the anatomical structure of the joint and establish whether a condition or an injury of cartilage, or other tissue is present and treat it without the loss of blood.
Such operations are meniscectomies, and include the recovery of the anterior cruciate ligament of the knee, chondromalacia patella, the recovery of the supraspinatus after rupture and many others.
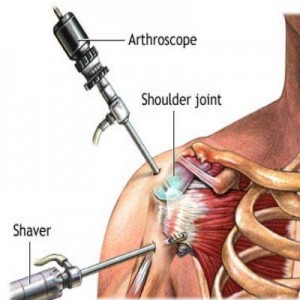
Arthroscopy of the shoulder is a minimally invasive surgical procedure in which through 3-5 small incisions around the area of the shoulder, the Surgeon gains access to all anatomic parts within the joint and around it.
There are plenty of surgical indications and the patient makes a much faster recovery than with an open surgical operation.
Conditions that can be dealt with arthroscopically are the rupture of the rotator cuff, damage of the labrum cartilage, acromial arthritis and so on.
The rupture of the supraspinatus tendon (partial or total) is one of the most frequent traumatic but mostly degenerative injuries of the shoulder area. When dealt with at the right time, and with all surgical indications present it can be treated by suturing of the ruptured tendon and the securing it to the sheath with the application of a special technique.
Acromioplasty is a surgical operation in which, with the use of special tools, the surgeon aims to broaden the anatomic area of the shoulder that has narrowed due to degenerative causes resulting in acute pain during arm movement.
It requires just a one day stay in hospital. The day after surgery, the patient wears a cast and leaves with directives on how to take care of the shoulder. A strict rehabilitation schedule should be followed for a few weeks.
The result is the relief from pain and the regained use of the shoulder.
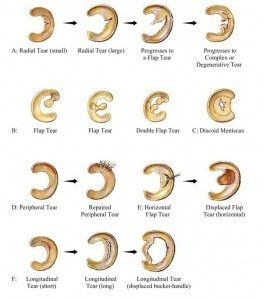
Meniscus tear
The meniscus (medial – lateral), is a semi-hard crescent shaped “cushion” that lies between the femur and the tibia. Its purpose is to absorb vibrations while walking or running, and the distribution of pressure on the cartilage area of the above mentioned bones.
It can be damaged during sport activity or otherwise from long term degeneration due to wear and tear.
A clinically and through scanning (imaging) diagnosed meniscus tear, needs to be dealt with conservatively as well as surgically. As soon as the condition exhibits surgical indications, planning of the operation and the recovery program should be made.
Not all meniscus injuries exhibit surgical indications. Some have relevant indications and others have full indications.
Injuries with full indications:
- extensive damage
- bad area (area with poor or no haematosis)
- injury with a free fragment in the joint
- professional sport activity
- mixed injuries (in conjunction with anterior cruciate ligament)
The damages can be acute (recent) or chronic (from the past). Nowadays, all meniscus conditions can be dealt arthroscopically with an operation called arthroscopy. Through two small incisions the surgeon inserts tools that are a few millimetres in diameter, as well as a camera connected to a monitor. A thorough inspection of all anatomic parts of the knee takes place and all damage is dealt with – in this case the meniscal tear.
The aim is to save and not remove meniscus, whenever feasible. The removal, or meniscectomy, can be partial or total, depending on the extent of the damage. It is worth mentioning that the bigger the part of meniscus removed the less the protection that is offered to the overlying and the underlying cartilages (femur and tibia)
The operation is performed with either an epidural or general anaesthesia. The surgical operation takes less than an hour and the patient is able to return home in the evening. The recovery is very quick and the return to previous daily activities is certain. The patient will have to use crutches for a small period of time followed by a short rehabilitation programme.
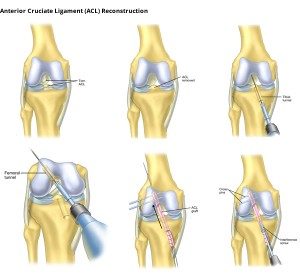
Anterior Cruciate Ligament ACL
The anterior cruciate ligament of the knee, lies within the centre of the joint and connects the femur to the tibia and is right in front of the posterior cruciate ligament. It is about 3 centimetres long and its function is to stabilize the joint in order to avoid shifting of the tibia in relation to the femur.
There is a high risk of injury, mainly during sports activities. The patient feels like something has snapped within the joint and a few hours later the knee becomes swollen and stiff due to a build-up of blood in it.
After collection of information and dedicated clinical tests, imaging inspection with x-rays and magnetic tomography (MRI) follows. In this way, the orthopaedic surgeon will have a clearer picture to verify the damage, along with other possible coexisting conditions of the anatomical structure of the knee.
The treatment is always arthroscopic. Since it is impossible to stitch the cruciate ligament, autografts (from the patient’s body) or synthetic grafts are used.
Following the surgical operation the patient needs to use crutches for a while and follow a strict rehabilitation process. How soon a patient can return to normal daily activities depends on the patient’s needs.